Menu
Close
Major Depressive Disorder, Part Two | Treatment and progress
Nov 9, 2022
This two-part series details the Canadian Mental Health Association (CMHA), Alberta Division’s three-year research project on Major Depressive Disorder (MDD); the impact MDD has on the lives of Canadians, how they cope with MDD, and what a brighter future looks like for Canadians with MDD – all through the lens of lived experience. In part two, we explore how MDD is typically treated and what can be done to improve the lives of Canadians with MDD.
Treatment
When it comes to treatment options for MDD, there is rarely an easy fix; while some forms of mental illness can be effectively managed by prescription medication, this form of treatment is part of a bigger picture for people with MDD. Wellness journeys tend to look more like a network or balance. While the balance differs from person to person, there are pillars of MDD treatment that tend to be more popular.
Medication
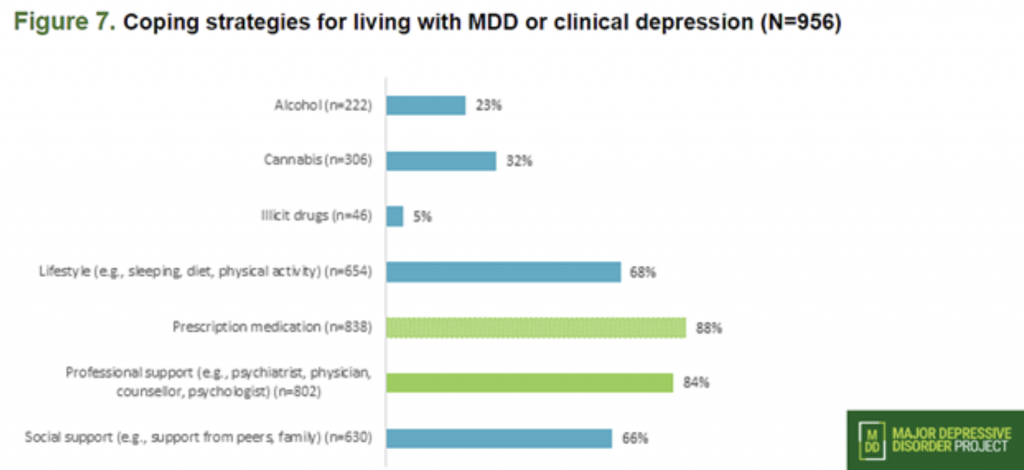
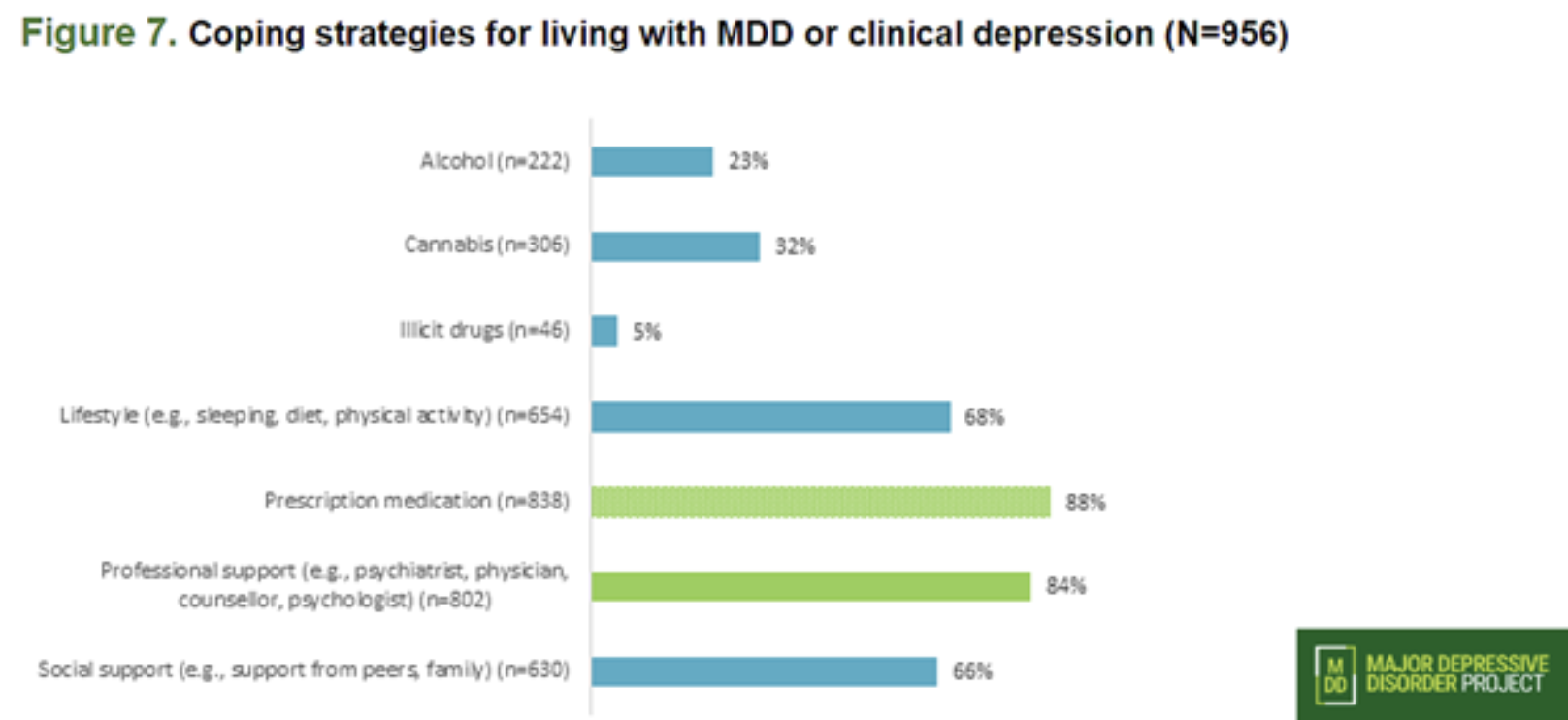
Prescription medication is not a cure-all for MDD – but that doesn’t stop it from being one of the most effective and popular forms of treatment. With 88 per cent of survey respondents citing medication as a coping strategy, MDD may not be entirely handled by medication, but it remains an important pillar in the treatment of MDD.
Professional Support
The second highest response for coping strategies was professional support, with physicians, psychiatrists, counsellors and psychologists being notable sources. One respondent was quoted as calling the healthcare system “…very isolating for people with mental disorders,” which reflected strongly in the survey. Affordability and finding professionals that were patient and well-informed regarding MDD were both identified as barriers.
Lifestyle
Maintaining healthy habits and behaviours is paramount to managing MDD and its symptoms. While proper sleep, diet, exercise, self-care and socializing are all part of a healthy lifestyle that can help alleviate some of the major symptoms of MDD, the disorder can actively sabotage the energy levels necessary to continue these activities. “Self-care is the first thing that goes [away],” one respondent said. “Even showering and brushing teeth is too much.”
This represents a compounding affect for people with MDD; positive lifestyle choices can represent too much of an energy investment, which can lead to a decay in self-maintenance and healthy habits, which can in turn exacerbate symptoms of MDD further. It becomes easy to see why people living with MDD are prone to spiralling.
Social Support
Social supports represented the fourth highest-ranked coping strategy, with 66 per cent of respondents receiving support from friends, family and peers. Stigmatization can get in the way of this strategy, with many respondents feeling the people around them wouldn’t understand or would treat them differently if they reached out. Like professional support, this strategy was also profoundly affected by the isolation of the pandemic.
Improving Lives Canada-Wide
Four major cornerstones of the research results became apparent when respondents were asked what progress looks like regarding MDD:
Improved accessibility for informed care
Respondents expressed a need for better accessibility for proper care. This included facets like access in rural communities, affordability of care and medication and for care to be specifically informed regarding MDD.
Fighting the stigma surrounding MDD
MDD being surrounded by stigma plays a major role in the lives of people that live with it. Raising awareness about MDD’s symptoms, what living with MDD looks like, and helping people to better understand how to support loved ones and peers that live with MDD are all vital steps to help fight the stigma.
Better workplace interventions to support employees living with MDD
Research results found that employers have an opportunity to be a cornerstone for improving the lives of people with MDD. Educational materials for employees, training for management and supervisory staff, written policies to help support employees and actively ensuring open dialogue to dispel stigma all rated highly as improvements respondents would like to see in their places of work. Respondents feared that MDD disclosure would affect their careers, felt guilt for any affect their diagnosis had on their work and judgment from coworkers was a major concern.
Continued research into the impact Covid-19 has had on Canadians with MDD
It is difficult to measure just how deeply the Covid-19 pandemic has affected Canadians living with MDD. Whether it be working from home and the stressors of returning to the office, being isolated from friends and family, or experiencing disruptions and general lack of accessibility to mental healthcare. The continued and active observation of these impacts are now an important part of understanding the realities of living with MDD.
Let’s work together
CMHA, Alberta Division conducted this work to better understand how MDD impacts the lives of Canadians and how to help mitigate those impacts. By continuing to raise awareness and amplifying the voices of Canadians living with MDD, advocating for the creation and accessibility of supports and resources most important to treatment, developing resources and calls to action for Canadian workplaces and further analyzing the pandemic’s effect on MDD, CMHA, Alberta Division is committed to a brighter future for Major Depressive Disorder and the Canadians experiencing it.